Treatment of Knee Injury
Objectives
The following objectives apply to this section of the web module.
1. Describe what medications that are commonly prescribed for knee injury with 90% accuracy.
2. State the types of imaging that would be ordered by a physician after knee injury with 90% accuracy.
3. Describe the content of a physical therapy evaluation for knee injury with 90% accuracy.
4. Describe common treatments that are prescribed by physical therapists after knee injury with 90% accuracy.
5. Formulate an initial exercise program for knee injury with 80% accuracy.
Please read the information below and try to figure out how our runner might be managed and what treatments she may receive.
1. Describe what medications that are commonly prescribed for knee injury with 90% accuracy.
2. State the types of imaging that would be ordered by a physician after knee injury with 90% accuracy.
3. Describe the content of a physical therapy evaluation for knee injury with 90% accuracy.
4. Describe common treatments that are prescribed by physical therapists after knee injury with 90% accuracy.
5. Formulate an initial exercise program for knee injury with 80% accuracy.
Please read the information below and try to figure out how our runner might be managed and what treatments she may receive.
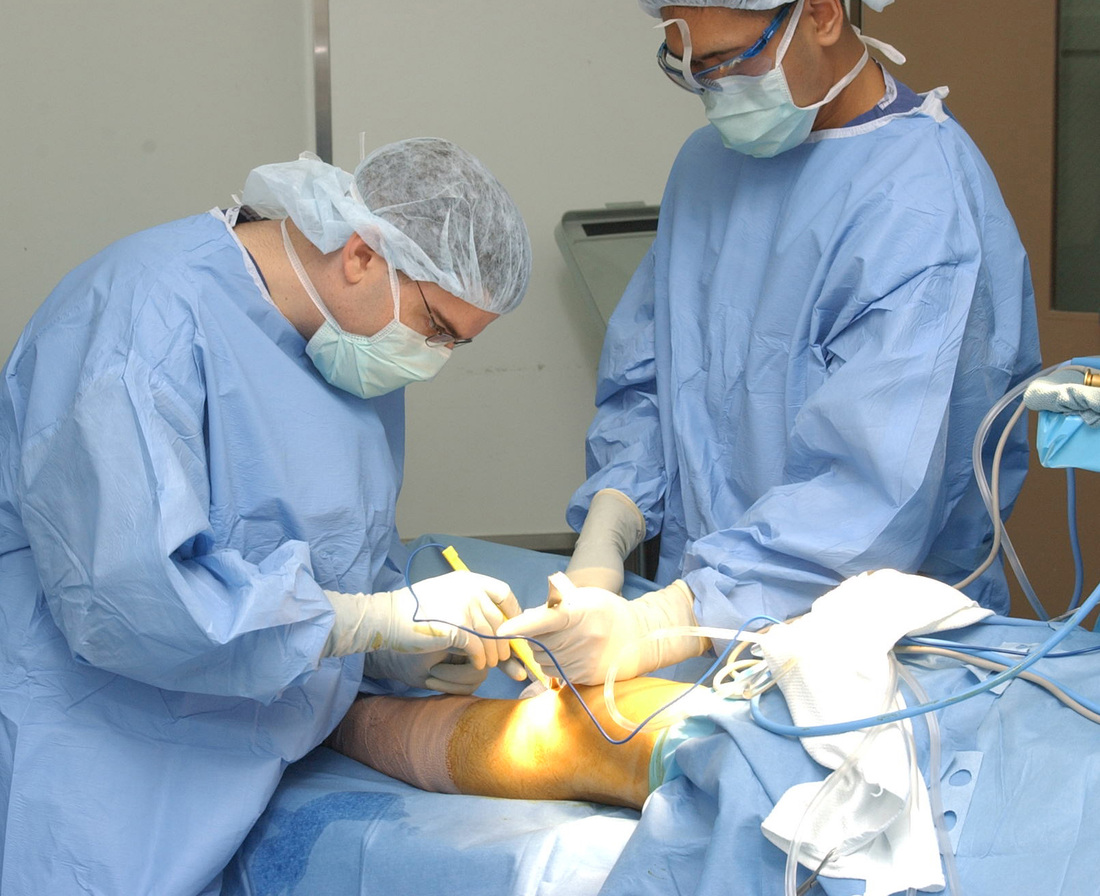
Medical Management of Knee InjuryAfter injury, your physician will look at the knee to check for any abnormalities such as swelling, tenderness, or inability to move the joint. The doctor may perform certain tests, called special tests, that look at specific structures within the joint in order to detect pathology. These tests will involve moving the joint in specific ways, or providing compression to the joint. Next, your physician may order imaging tests (x-rays, or MRI's) to confirm the diagnosis made through the physical exam, to diagnose problems with the bone or soft tissue, respectively.
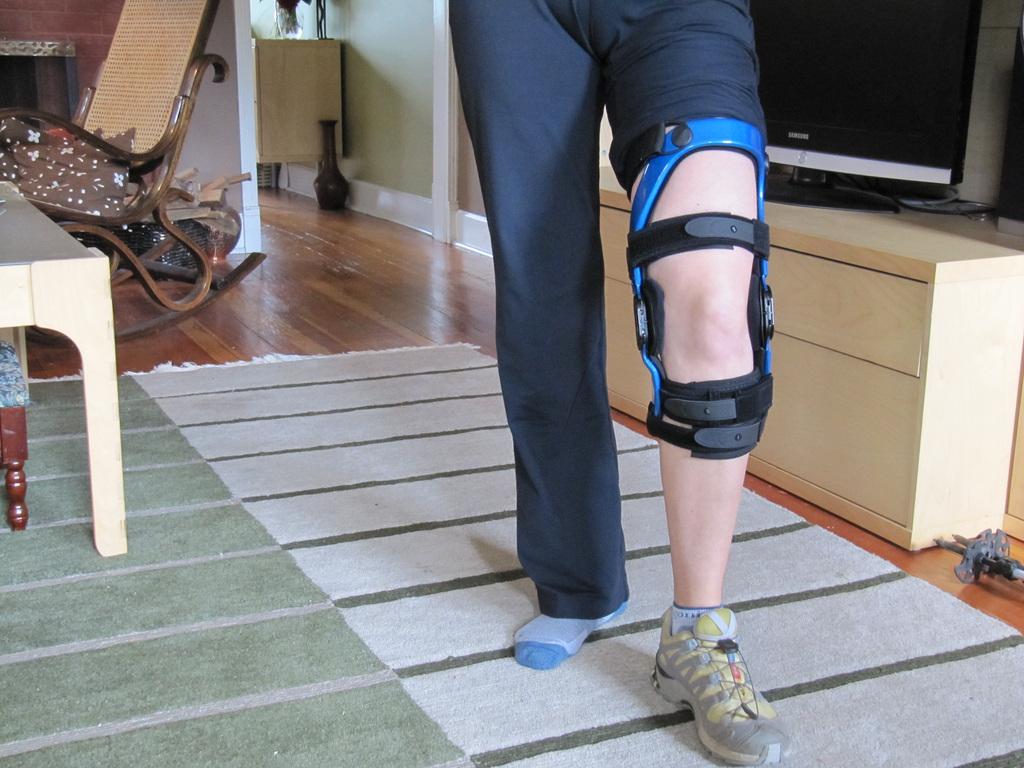
(Greisamer and Kelly, 2007, August) Initial management of knee injury will from a medical standpoint will focus on reducing inflammation, using a technique known as RICE (Rest, Ice, Elevate, and Compress) (Greisamer and Kelly, 2007, August)). These strategies may include: decreasing the amount of weight someone may put on the injured limb, immobilizing the joint, elevating the limb to decrease swelling, using an elastic bandage, or using ice for 20 minutes an hour to decrease swelling (ibid). Anti-inflammatory medications such as NSAIDS (Non-Steroidal Anti-Inflammatory Drugs) or certain types of pain medications may be prescribed for inflammation and pain management, respectively. The doctor may also prescribe physical therapy as a form of conservative management, depending on the type of injury. If conservative management techniques, such as the techniques noted above do not work, then surgery may be undertaken to repair the affected structure. |
|
Physical Therapy Management of Knee InjuryEvaluation
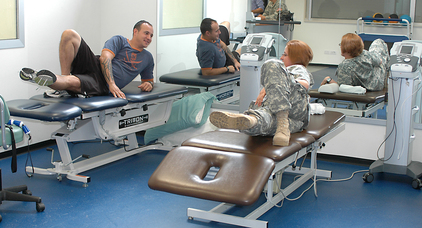
Physical Therapists manage knee injuries on a regular basis. Please watch the video to the right to hear a physical therapist talk briefly about the evaluation of the knee joint. |
|
|
Overall Management
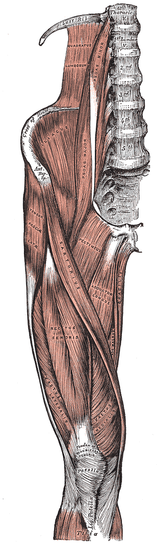
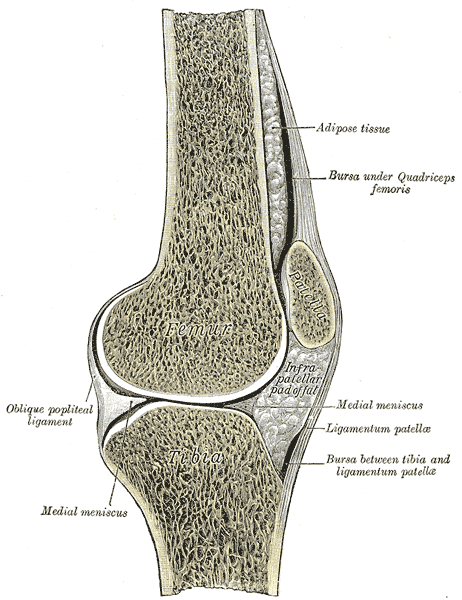
Physical therapy management of knee injury will dependent on the phase of injury, however, the overall goal of physical therapy is to return the person to their normal, daily activities or sports, and to educate the patient on prevention of further injury. Throughout the course of treatment, the therapist will be focused on return of range of motion, strength, reduction in pain, and return to function. In the first or acute phase of injury, the physical therapist will be concerned with the management of inflammation, knee pain, and swelling through use of ice, ultrasound, compression, or electrical stimulation. Another focus will be on increasing range of motion by using exercises that increase bending and straightening of the leg. Stretching exercises may also be prescribed during this phase depending on the type of injury that the patient has. These exercises are given to increase the available range of motion in the muscles to prevent further injury. As the pain begins to lessen, inflammation decreases, and range of motion increases, the physical therapist will add specific strengthening exercises for the muscles that surround the knee and hip joint so that the joint is better supported. The physical therapist will focus on the primary muscles that: bend the hip (rectus femoris and iliopsoas), bring the leg towards the body (the hip adductors (adductor magnus, longus, and brevis; pectineus, and gracilis), bring the muscles away from the body (hip abductors (gluteus medius and tensor fasciae latae), the knee flexors (hamstrings (semembranosus and semitendinosus, and biceps femoris), and the knee extensors (quadriceps (rectus femoris, vastus medialis obliqius, vastus lateralis, vastus intermedius), depending on the type of injury (Brunnstrom, 1996). These muscles are noted in the diagram to the right. Exercises will be progressed as strength builds and pain lessens by progressing from body weight resistance to adding weights or elastic bands for resistance. Exercises are generally progressed when three sets of ten repetitions of the exercises become easy, starting with lower amounts of weight or resistance, and progressing to higher levels of weight or resistance. The initial amount of weight is determined by having the patient try to perform 8-10 repetitions of the exercise with a specific weight or resistance. If the patient is able to exceed this without fatigued, the weight or resistance is increased, until the patient is fatigued after 8-10 repetitions. If the patient does not achieve 8-10 repetitions due to fatigue or pain, then the weight or resistance is decreased until the patient can comfortably perform 8-10 repetitions to fatigue. After working on specific strengthening exercises, and once the patient is pain free with normal range of motion, the therapist will focus on activities to return the person to sport or to daily activities by prescribing certain exercises or movements that simulate daily activities. These movements could include quick changes of direction, increasing speed and then decreasing speed, balance activities, or stair climbing. After the patient is pain free, has adequate strength for desired activities, has adequate range of motion, and can function normally, the patient will be discharged from physical therapy services. The video to the right will demonstrate some exercises used at the start of rehabilitation of the knee from each of the below knee injuries. This video is not meant to substitute for professional medical advice, or consultation with a physical therapist on specific exercises that will benefit you. Since each patient is different, it is recommended that you seek medical advice from a qualified medical professional or physical therapist should you experience an injury to your knee joint. Management of Specific Injuries Meniscal Tears Rehabilitation of a meniscal tear will begin with conservative management, as long as the patient's knee is not locked (the patient cannot fully extend and is stuck in a large degree of bending). If the patient's knee is locked, it is possible that the patient may need surgery. Conservative (non-surgical) management of the tear will focus on rest, ice, compression, and elevation, as well as other modalities for pain management such as electrical stimulation or ultrasound. As pain is being managed, focus will be on increasing range of motion as well as on isometric exercises of the hamstring and quadricep (tightening the muscle). Additional hip exercises may be used to begin strengthening the muscles surrounding the hip and knee. As the patient becomes pain-free, resistance will be added to the exercises to strengthen the knee flexors and extensors. Furthermore, the patient will be progressed to weight bearing exercises such as squatting and wall slides. Finally, the patient will focus on a return to sporting activities with agility and cutting drills. If surgery is needed, rehabilitation after surgery will focus on a gradual increase in range of motion and strengthening with gradual return to activity, however, will depend on the type of surgery performed, and should be directed by a qualified medical professional. Patellofemoral Pain Syndrome Early in rehabilitation, focus will be on decreasing the inflammation around the knee, using rest, ice, compression, and elevation. Foot orthotics may also be attempted if the patient is noted to over-pronate during running. Further rehabilitation of this problem depends on the cause of this problem. If the problem is due to tightness of the tensor fasciae latae, and lateral musculature and ligaments focus will be on stretching this muscle. In addition, taping may be used to position the kneecap in the proper position. The therapist may employ joint mobilization of the kneecap to get the kneecap moving in the proper alignment. If the problem is more related to strength of the muscles that straighten the knee, focus will be on strengthening these muscles using exercises such as quad sets, shallow squatting, shallow wall slides, hip adduction, and short arc quadricep extensions. These exercises will be guided by the patient's pain level. In addition, the muscles that straighten the hip, bring the leg out an end, and bend the hip may also be strengthened to improve the position of the femur during standing and walking (McGee, 2009). In addition to strengthening exercises, the therapist may use a tool known as biofeedback. Biofeedback detects the recruitment of the quadriceps muscles and provides a visual (seeing) or auditory (hearing) stimulus to let the patient know if the muscle is contracting. This tool may be used to help patients know if they are contracting the correct muscle as they try to build strength. Muscle Strain In the early phase, a strategy of protection from further injury, rest, ice, compression, elevation, and modalities will be used to manage pain. After the patient is relatively pain free, progression to strengthening and agility drills will become the focus of therapy (McGee, 2009).
Ligament Sprain
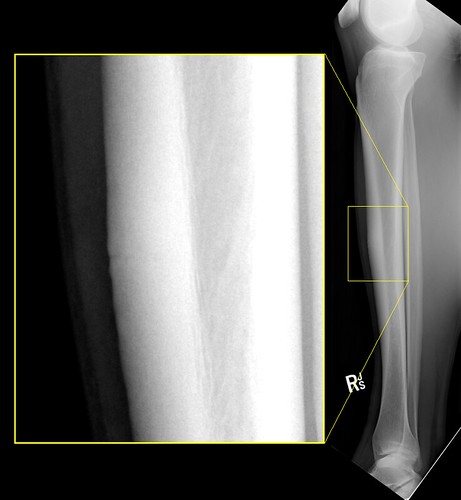
After full range of motion of the knee has been achieved, light resistance exercise with higher amounts of repetitions will be added to begin endurance. These exercises will first take place in sitting (long arc quads and hamstring curls) and then will be progressed to wall slides and step up exercises. After muscular endurance has been established, the repetitions will decrease and the amount of resistance will increase to build strength, both concentrically (lifting) and eccentrically (lowering). In the final stages of the program, focus will be on building power and neuromuscular control to ensure that joint control of motion is sufficient for all activities (McGee, 2009). Iliotibial Band Syndrome Specific treatment for this syndrome is focused on reducing inflammation at the knee joint by use of modalities such as ice, ultrasound, or electrical stimulation. These modalities, however, will not result in a permanent decrease in pain or inflammation, unless the length of the muscle is increased. The focus of physical therapy will be on manual therapy to increase the length of the tensor fasciae latae and iliotibial band, as well as increasing the strength of the hip abductors and hip extensors. Stress Fractures In low risk fractures, symptomatic management of pain will occur with various modalities such as ice, ultrasound, or pulsed electromagnetic therapy (McGee, 2009). A gradual loading program, guided by pain, will be used to rent the patient to running (McGee, 2009). This program starts with walking, progresses to walking and jogging, and then finally progresses to running. For more details on a graduated loading program, please see this link. In high risk fractures, such as in the neck of the femur, anterior cortex of the tibia, medial malleolus, talus, navicular, fifth metatarsal, and great toe sesamoids, rest and immobilization are the standard of care until the fracture is healed (McGee, 2009). |
Above video by Nancy Smith, PT, DPT, GCS. Permission is given for re-use of this video for educational purposes. No commercial use is allowed.
Tibial Stress Fracture, by P^2 - Paul on Flickr, Creative Commons License
|
Self Check Quiz
|
References
Content written by Nancy Smith, PT, DPT, GCS; images courtesy of wikimedia commons.
1. Brunnström, S. (1996). Brunnstrom's Clinical Kinesiology revised by Smith K, Weiss E, and Lehmkuhl D. Philadelphia, PA: Davis. 2. Greisamer, RP and Kelly FB (2007, August). Knee and lower leg. http://orthoinfo.aaos.org/menus/leg.cfm. Retrieved April 1, 2013 from http://orthoinfo.aaos.org/menus/leg.cfm.
3. Magee, D. J., Zachazewski, J. E., & Quillen, W. S. (2008). Pathology and intervention in musculoskeletal rehabilitation. Saunders.
4. Salter, R. B. (1999). Textbook of disorders and injuries of the musculoskeletal system: an introduction to orthopaedics, fractures and joint injuries, rheumatology, metabolic bone disease, and rehabilitation. Williams & Wilkins.
1. Brunnström, S. (1996). Brunnstrom's Clinical Kinesiology revised by Smith K, Weiss E, and Lehmkuhl D. Philadelphia, PA: Davis. 2. Greisamer, RP and Kelly FB (2007, August). Knee and lower leg. http://orthoinfo.aaos.org/menus/leg.cfm. Retrieved April 1, 2013 from http://orthoinfo.aaos.org/menus/leg.cfm.
3. Magee, D. J., Zachazewski, J. E., & Quillen, W. S. (2008). Pathology and intervention in musculoskeletal rehabilitation. Saunders.
4. Salter, R. B. (1999). Textbook of disorders and injuries of the musculoskeletal system: an introduction to orthopaedics, fractures and joint injuries, rheumatology, metabolic bone disease, and rehabilitation. Williams & Wilkins.